Does it feel like you’re sitting on a hot poker every time you sit on a hard surface? Do you squirm around in long meetings, having to shift from one butt cheek to the other to try and relieve the pain? You may be suffering from coccydynia, or tailbone pain. But don’t lose hope! There is treatment available.
Most people understand why their tailbone might hurt after a hard fall on the rear, but what about tailbone pain that seems to come out of nowhere and never goes away? This happens more often than you might think (especially among women and those with other pelvic conditions like pelvic pain), and it can be linked to problems with the pelvic floor. Tight muscles, sitting position, and a history of injuries to the area can all play a role.
How can I tell if I have tailbone pain?
The tailbone, or coccyx, is the very bottom of the column of bone that includes your spine and sacrum. It’s a small, roughly triangular bone that attaches to your sacrum at a little joint called the sacrococcygeal joint.
You can feel the tip of your own tailbone if you press along the bone that goes down the upper part of your buttcrack and feel where it ends – usually an inch or two above the anus. If this area hurts, you officially have coccydynia!
Pain in the tailbone area usually presents in one of two ways. Sometimes the pain is concentrated around the tip of the bone, where it might feel like there is a single, sharp tender point that hurts when it comes into contact with a surface (like a hard chair). Other people have more pain around the sacrococcygeal joint, which is a little higher up and may feel a bit more spread out. This second type of pain is often the worst when standing up after sitting for a while, when the joint moves a bit. You may be experiencing both!
What causes tailbone pain?
Tailbone pain can affect people of all ages and all genders. Common causes of tailbone pain are trauma (including a fall or childbirth), prolonged sitting on a hard surface, and pelvic floor muscle tension.
Fall or injury
If you fall on your behind, you can either sprain the joint, or actually fracture the bone. Depending on how you land, the tailbone can be bent too far forward or back, or may be pushed off center toward the left or the right.
If your pain started with a hard fall or some other type of physical trauma, and/or if it persists past the 6-8 week mark and isn’t responding to conservative treatment, it’s best to get imaging (like an X-ray) performed to help identify the cause and a treatment plan.
Pregnancy or postpartum
Tailbone injury can also occur during vaginal childbirth, if your baby’s head presses hard enough (and/or quickly enough) against the bone as it is coming through the birth canal. During pregnancy, body shape and posture changes can make the tailbone more mobile and sensitive.
The whole pelvic region tends to be sore right after delivery, so it can be hard to tell if the case is the tailbone or something else. If pain is severe and persistent after a couple of weeks postpartum and seems further back than the vagina, schedule a visit with a pelvic floor physical therapist who can help assess and support your recovery.
Prolonged sitting
Sore tailbone from sitting? You’re not alone; it’s a common cause of tailbone pain. Since the tip of the bone is pretty pointed, and we don’t have much natural padding there, sometimes just the pressure of a surface on the bone can create an injury to the soft tissue. In this case it is particularly important to try and sit on softer surfaces, and to avoid positions that put further pressure on this area.
If you sit in a more slumped position with your butt “tucked under”, there is more pressure on the tailbone. If you sit a bit more upright, with the weight more on the sit bones, the pressure on the tailbone should decrease. Sometimes placing a small pillow at the small curve of the lower back is helpful in maintaining this position. Sitting up in bed for prolonged periods is a common cause of tailbone pain – it is very difficult to maintain good posture in bed.
A physical therapist can help you troubleshoot your chair setup and sitting posture to help you get more comfortable and prevent future issues!
Pelvic floor tension
The pelvic floor muscles also connect directly to the tailbone. If these muscles are too tight, especially for longer periods of time, they can tug the tailbone into a more tucked position or over to one side and also cause pain. The gluteus maximus, or largest glute muscle, also connects to the coccyx, so if you are doing heavy weight training of this muscle you may also experience some discomfort in this area.
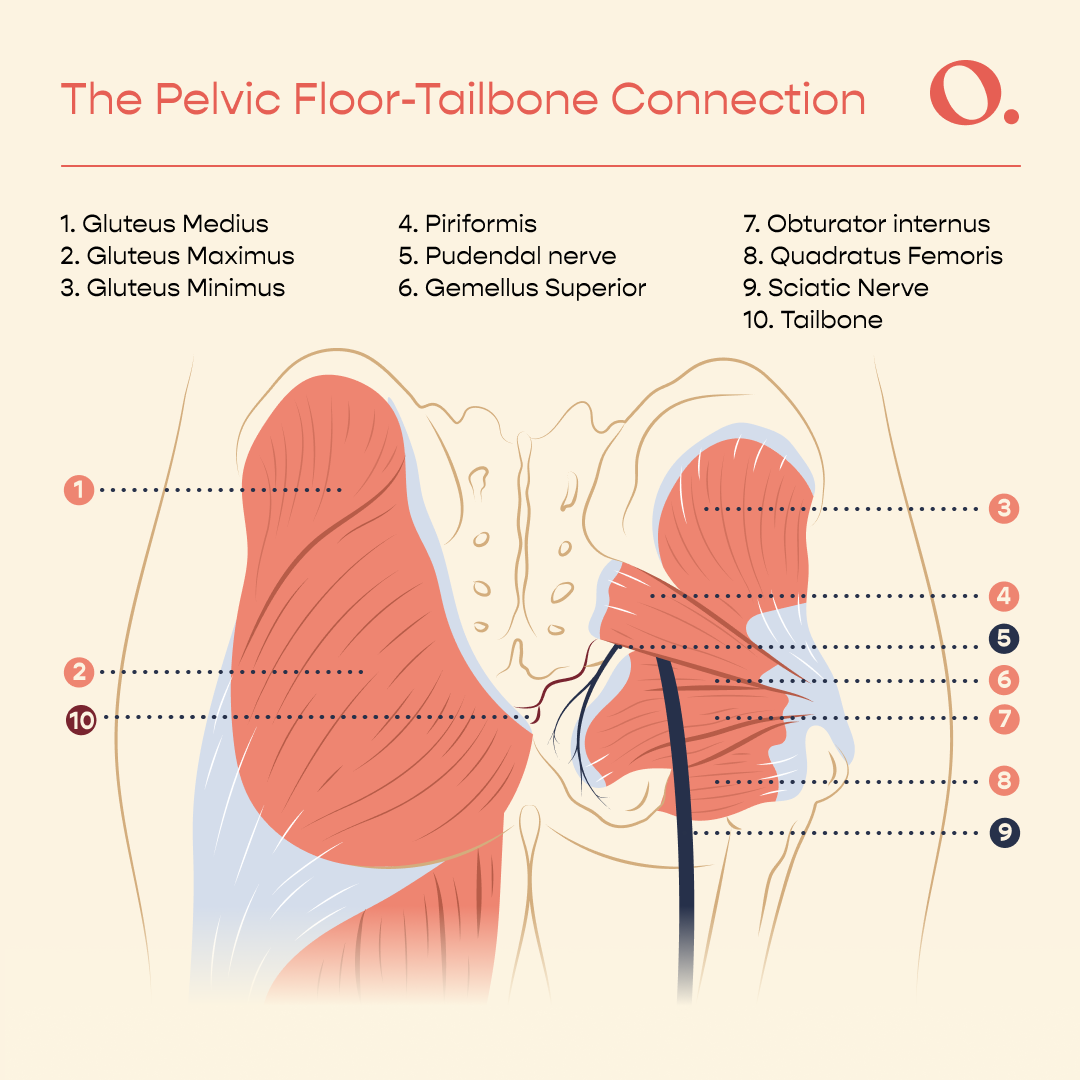
If you can poke around the muscles on either side of the tailbone and they feel tight and tender, that’s a clear way to tell that your issue may be pelvic floor-related.
Other signs of potential pelvic floor tension include:
- Pain with intercourse or other types of penetration (inserting a tampon, getting a pap smear)
- Pain or difficulty with bowel movements
- Frequency and urgency with urination
- Pain in other nearby areas like the sit bones, perineum, bladder, rectum, anus, vulva, or testicles in AMAB folks.
Health care providers who don’t specialize in pelvic health are often less aware of this type of tailbone pain, and may not offer appropriate treatment – in this case, pelvic floor physical therapy is usually the best bet!
What are the best treatments for tailbone pain relief?
From cushions to physical therapy, there are several ways to find relief depending on what's causing your pain.
Adjust your sitting posture
If sitting is aggravating your tailbone, small changes can make a big difference. Sit upright with your weight on your sit bones rather than tucked under, and try a cushion with a tailbone cutout for extra relief.
At-home stretches
Think your tailbone pain might be pelvic floor-related? Try these stretches to help lengthen and relax the muscles attaching to your tailbone.
Figure 4 Stretch
To stretch out the hip and pelvic floor muscles that attach to the tailbone, try this stretch! Cross one ankle over the opposite knee, and then press the crossed knee away from you until you feel a stretch in your glute. You can do this on your back (‘supine’), sitting in a chair, or standing up.
Wide Leg Child’s Pose
With knees comfortably apart, bring hips back and let your upper body relax toward the floor. Breathe deeply into your pelvis.
Happy Baby
While lying on your back, grab your feet, knees, or the backs of your thighs, and bring your knees toward your armpits until you feel a stretch between your legs and hips. Breathe deeply and try to relax your pelvic floor and glutes.
Pelvic floor physical therapy
Pelvic floor physical therapy is one of the most effective treatments for tailbone pain, especially when the cause is muscle tension, a history of childbirth, or pain that hasn't responded to other treatments. A pelvic floor PT can assess your posture, release tight muscles, and build a plan specific to your situation.
Frequently asked question: Should I use a donut cushion?
If you have broken your tailbone, you may be given an inflatable “donut” cushion to sit on during your recovery. While they may take pressure off the tailbone, they are generally not very comfortable to sit on overall, and can make good posture difficult.
Often, what is more comfortable is a larger cushion that supports the whole pelvis, with a little cutout in the tailbone region. Our clinicians love and recommend these: Wedge Seat Cushion with Coccyx Cut Out and Tush Cush Coccyx Cushion.
Medical treatment for severe cases
While conservative care is usually effective, for severe cases, there are other treatment options available. They can include medications to reduce muscle spasm, nerve block injections, electric shock wave therapy, and for the most stubborn cases, surgery, to remove part of the tailbone.
Often, pelvic floor therapy is prescribed alongside these more intensive treatments, to help assist with recovery and reduce risk factors that could cause the pain to come back (Scott et al 2017).
Ready to find relief from your tailbone pain?
Tailbone pain is frustrating, but the good news is you don't have to just live with it. Whether your pain is from an old injury, prolonged sitting, or pelvic floor tension, Origin’s pelvic floor physical therapists can help you find the cause and get you back to sitting and moving comfortably. Schedule your evaluation today!
Sources
Blanco-Díaz et al. "Physiotherapy approaches for coccydynia: evaluating effectiveness and clinical outcomes." BMC Musculoskeletal Disorders, 26 (2025). https://doi.org/10.1186/s12891-025-08744-3.
Nathan, S T et al. “Coccydynia: a review of pathoanatomy, aetiology, treatment and outcome.” The Journal of bone and joint surgery. British volume vol. 92,12 (2010): 1622-7. doi:10.1302/0301-620X.92B12.25486
Scott et al. "The Treatment of Chronic Coccydynia and Postcoccygectomy Pain With Pelvic Floor Physical Therapy." PM&R, 9 (2017). https://doi.org/10.1016/j.pmrj.2016.08.007.
Sidiq et al. "Effectiveness of physical therapy interventions for coccydynia: a systematic review with a narrative synthesis." Archives of Physiotherapy, 15 (2025): 77 - 89. https://doi.org/10.33393/aop.2025.3233.





