Understanding the outside of your body is one thing: your height, weight, shoe size… But have you ever wondered what’s happening on the inside? A dual-energy X-ray absorptiometry, or DEXA, scan can tell you all about things under your skin. Read on as we discuss DEXA scan basics and beyond, including what a DEXA scan is, how to understand your scan results, and how getting a DEXA scan can benefit your pelvic floor health.
What is a DEXA scan?
A DEXA, or DXA, scan is an imaging test that measures your body’s three main components: bone mass, fat mass, and lean mass. Similar to a standard X-ray, a DEXA scan is quick, non-invasive, and pain-free. It uses low-dose X-rays that provide a detailed analysis of your body composition and bone density, which is why it’s also called a bone density test.
What does a DEXA scan measure?
While at-home smart scales do their best, a DEXA scan tells you a lot more about your body than a scale or a typical X-ray. A DEXA scan looks at your:
- Bone mineral density (BMD): Dense bones contain more calcium and other minerals and are less likely to break or fracture. Knowing your BMD can help your healthcare provider assess your risk of osteoporosis and its precursor, osteopenia.
- Fat mass and body fat percentage: Understanding where your body carries fat is just as important as knowing how much there is. A DEXA scan measures your visceral fat, or the amount of fat around your organs, and excessive visceral fat is a risk factor for several diseases. Dexa scans also measure whether you carry more fat around your hips or midsection, and your total body fat percentage.
- Lean mass: Lean mass includes everything in your body that isn’t bones or fat tissue, including muscles, organs, and connective tissue. A DEXA scan looks at how much muscle mass you have in different parts of your body, alerting you to possible imbalances or asymmetry.
How is a bone density test done?
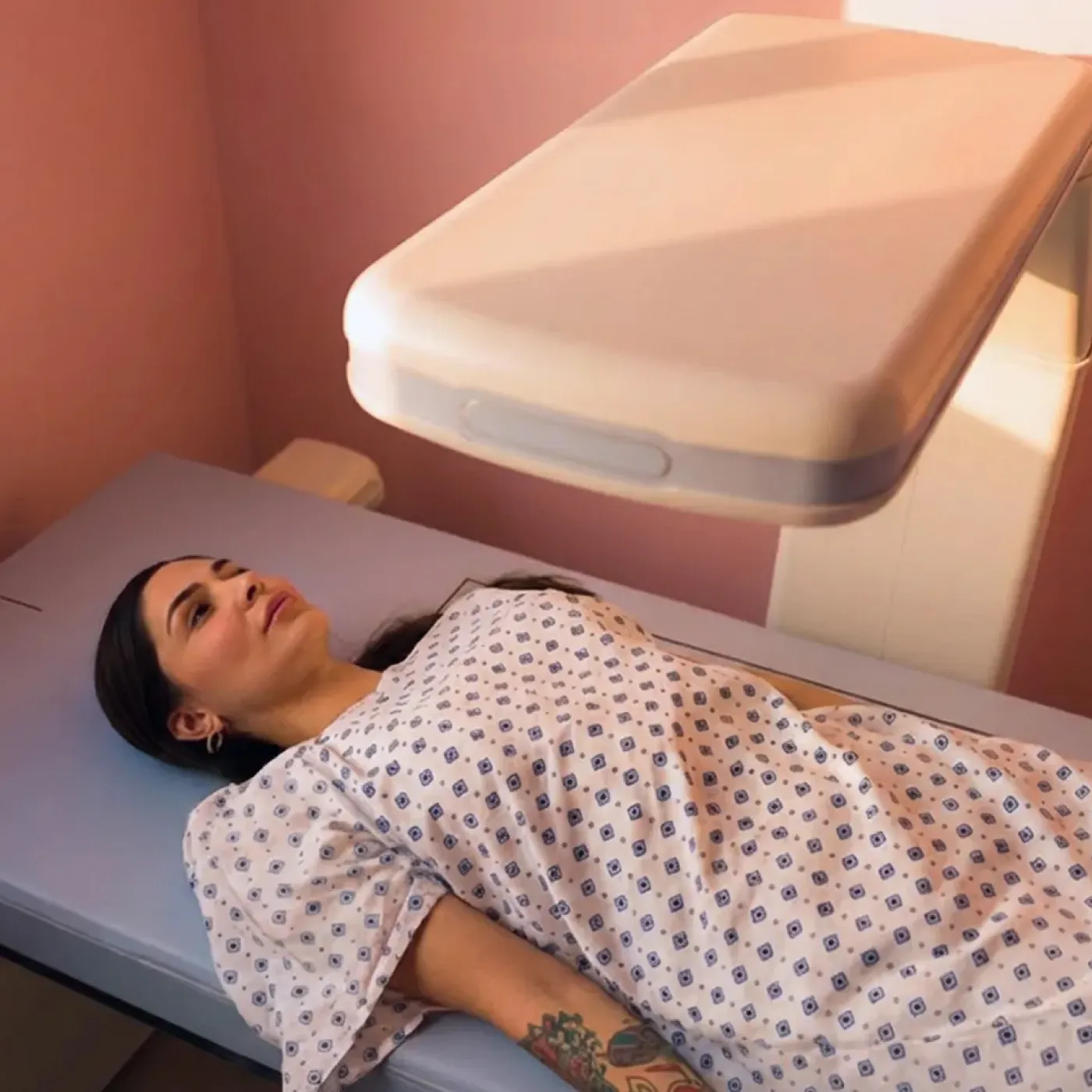
Testing your bone density with a DEXA scan is quick, easy, and painless. Unlike an MRI, no enclosed tube, injections, or needles are necessary! Instead, you’ll lie still on your back on a padded table. A scanning arm will pass slowly over your body, and, at the same time, another scanning machine will pass under you. The test usually takes about 10-30 minutes.
Who should get a DEXA scan?
A DEXA scan is a useful tool for anyone interested in learning about their body at a deeper level. Your body composition (lean mass percentage, fat mass percentage, and bone density) can change a lot over time. In particular, things like GLP-1 medication use, menopause, and aging can impact your body’s makeup and bone density, which can affect your musculoskeletal (MSK) and pelvic floor health. DEXA scans can help you understand and monitor these changes over time.
Consider asking your healthcare provider for a referral for a bone density DEXA scan if you:
- Are aged 65 or older
- Have a family history of osteoporosis
- Are going through perimenopause or have reached menopause
- Are taking a GLP-1 medication
- Weigh less than 127 pounds or have a body mass index (BMI) less than 18.5
- Have lost your period for 1+ years before age 42
- Currently smoke cigarettes
Certain medical conditions such as an eating disorder, rheumatoid arthritis, inflammatory bowel disease (IBD), among others, can also cause a loss of bone density. If you have or had one or more of these conditions, your provider may also recommend a DEXA.
How often should you get a bone density test?
While side effects of DEXA scans are slim to none, it’s important to know that these tests do use small amounts of radiation. To reduce your exposure to radiation, most providers recommend a DEXA scan no more often than once every one to two years.
What do my DEXA scan results mean?
Before we dive into the details, it’s important to understand that DEXA scan results aren’t a diagnosis or a permanent label! They’re just a snapshot of where your body composition and bone density stand today. Your body and bones respond to exercise, diet and nutrition, and corrective physical therapy when needed. With that in mind, let’s discuss the correct interpretation of DEXA scan results.
How to read bone density results
A DEXA scan will give you your bone density results in numbers called T-scores and Z-scores.
Understanding T-scores
Your T-score is a measure of how your bone density compares to a healthy adult of the same sex at “peak” bone density age, usually around age 30. Your DEXA scan will include a T-score if you’re approaching menopause or postmenopausal. Here’s how a T-score is categorized:
- -1.0 and above: Normal bone density
- -1.0 to -2.5: Low bone density, or osteopenia
- -2.5 and below: Very low bone density, possible osteoporosis
Understanding Z-scores
Your Z-score compares your bone density to others of your same age, sex, weight, and race. Z-scores are useful measures if you’re premenopausal, and, similar to T-scores, a higher number means you have a higher bone density.
DEXA scan body composition results
Beyond bone density measurements, DEXA scans can also provide detailed information about how much muscle and fat your body is carrying. This information may be useful if you’re tracking your fitness levels, recovering from an injury, on a weight loss journey, or just curious about your body! A scan can tell you your:
- Total body fat percentage
- Visceral adipose tissue, or fat around your organs
- Distribution of muscle and fat in your arms, legs, and trunk
- Side-to-side differences, if you have muscle asymmetry or imbalance
What a DEXA scan reveals about your musculoskeletal health
Your MSK system refers to the structures that give your body stability and allow you to move: your bones, muscles, and connective tissue. Taking care of your MSK system (i.e., maintaining bone density and muscle mass) is essential to living a long, healthy life. Strong bones help you stay mobile and fracture-free, and strong muscles support your joints and daily function. Maintaining both helps you increase your healthspan, or the period of life you spend in good health.
Periodic DEXA scans allow you to monitor your MSK system and how it changes over time. Staying proactive about your MSK health is particularly important for women and those assigned female at birth, as people born with ovaries are especially vulnerable to losing bone and muscle strength as they age. DEXA scans show you how strong your MSK foundation is today, so you can make any needed changes for a healthy tomorrow.
DEXA scans and your pelvic floor
Your pelvic floor muscles (PFM) don’t operate in a vacuum; they’re (a very important!) part of your MSK system. Bone density, body composition, and muscle imbalances can all affect your pelvic floor function. Here’s how DEXA scans can keep you in the know:
- Monitor bone strength: Urinary incontinence is the most common pelvic floor symptom, and low bone strength is associated with an increased risk of urinary incontinence in postmenopausal women.
- Track body fat levels: Carrying extra body fat around your midsection and pelvis can cause chronic strain, stretching, and weakening of the PFM. This can lead to pelvic floor dysfunction, especially stress urinary incontinence.
- Stay ahead of sarcopenia: Without proper nutrition and strength training, both menopause and rapid weight loss (such as that resulting from GLP-1 use) can increase your risk of losing skeletal muscle mass and strength, called sarcopenia. Sarcopenia can impact how well your PFM function and possibly lead to pelvic floor dysfunction.
- Notice muscle imbalances: Your PFM are deeply connected to muscles that support and control your posture and stability. Weakness or asymmetry in your back and core muscles can affect your PFM, possibly leading to pelvic floor symptoms.
While a DEXA scan may show muscle imbalances or weakness, these results may not always impact your pelvic floor or cause symptoms! A pelvic floor physical therapist can interpret your DEXA scan and figure out which scan results are most relevant to your pelvic floor health.
How your pelvic floor PT can use DEXA data
A DEXA scan gives you heaps of detailed information about your body… but what do you do with all that info? Here’s where a pelvic floor physical therapist can help! Origin’s expert clinicians can review your scan results, using the data to provide personalized and proactive care. From joint pain and body aches to surgery prep and recovery, our team is here to keep you balanced and feeling your best. Schedule your evaluation today.
Sources
“Bone Density Scan: MedlinePlus Medical Test.” Medlineplus.gov, 16 Sept. 2021, medlineplus.gov/lab-tests/bone-density-scan.
Raheem, Javeria, et al. “Visceral Adiposity Is Associated with Metabolic Profiles Predictive of Type 2 Diabetes and Myocardial Infarction.” Communications Medicine, vol. 2, no. 1, 1 July 2022, pp. 1–7, www.nature.com/articles/s43856-022-00140-5, https://doi.org/10.1038/s43856-022-00140-5.
Krugh, Marissa, and Michelle D. Langaker. “Dual Energy Xray Absorptiometry (DEXA).” PubMed, StatPearls Publishing, 2024, www.ncbi.nlm.nih.gov/books/NBK519042.
Wright, Vonda J., et al. “The Musculoskeletal Syndrome of Menopause.” Climacteric: The Journal of the International Menopause Society, vol. 27, no. 5, 30 July 2024, pp. 1–7, pubmed.ncbi.nlm.nih.gov/39077777/, https://doi.org/10.1080/13697137.2024.2380363.
Meyer, Isuzu, et al. “Pelvic Floor Disorder Symptoms and Bone Strength in Postmenopausal Women.” International Urogynecology Journal, vol. 31, no. 9, 29 Feb. 2020, pp. 1777–1784, https://doi.org/10.1007/s00192-020-04254-z. Accessed 28 Sept. 2023.
Kuutti, Mari A, et al. “Association of Body Composition with the Symptoms of Pelvic Floor Disorders in Middle-Aged Women: A Longitudinal Study.” Menopause the Journal of the North American Menopause Society, 3 June 2025, journals.lww.com/menopausejournal/fulltext/9900/association_of_body_composition_with_the_symptoms.468.aspx, https://doi.org/10.1097/gme.0000000000002572. Accessed 20 June 2025.
Rossi, Giada, et al. “Muscle Loss and GLP-1R Agonists Use.” Acta Diabetologica, 7 Nov. 2025, https://doi.org/10.1007/s00592-025-02611-2.
Grosman, Yacov, and Leonid Kalichman. “Bidirectional Relationships between Sarcopenia and Pelvic Floor Disorders.” International Journal of Environmental Research and Public Health, vol. 21, no. 7, 5 July 2024, p. 879, https://doi.org/10.3390/ijerph21070879.
Atkın, Ilknur. “The Pelvic Floor and Posture: Exploring the Foundations of Functional Balance.” BAU Health and Innovation, vol. 3, no. 2, Aug. 2025, pp. 91–98, pdf.journalagent.com/bauhi/pdfs/BAUH-62681-REVIEW-ATKIN.pdf, https://doi.org/10.14744/bauh.2025.62681.