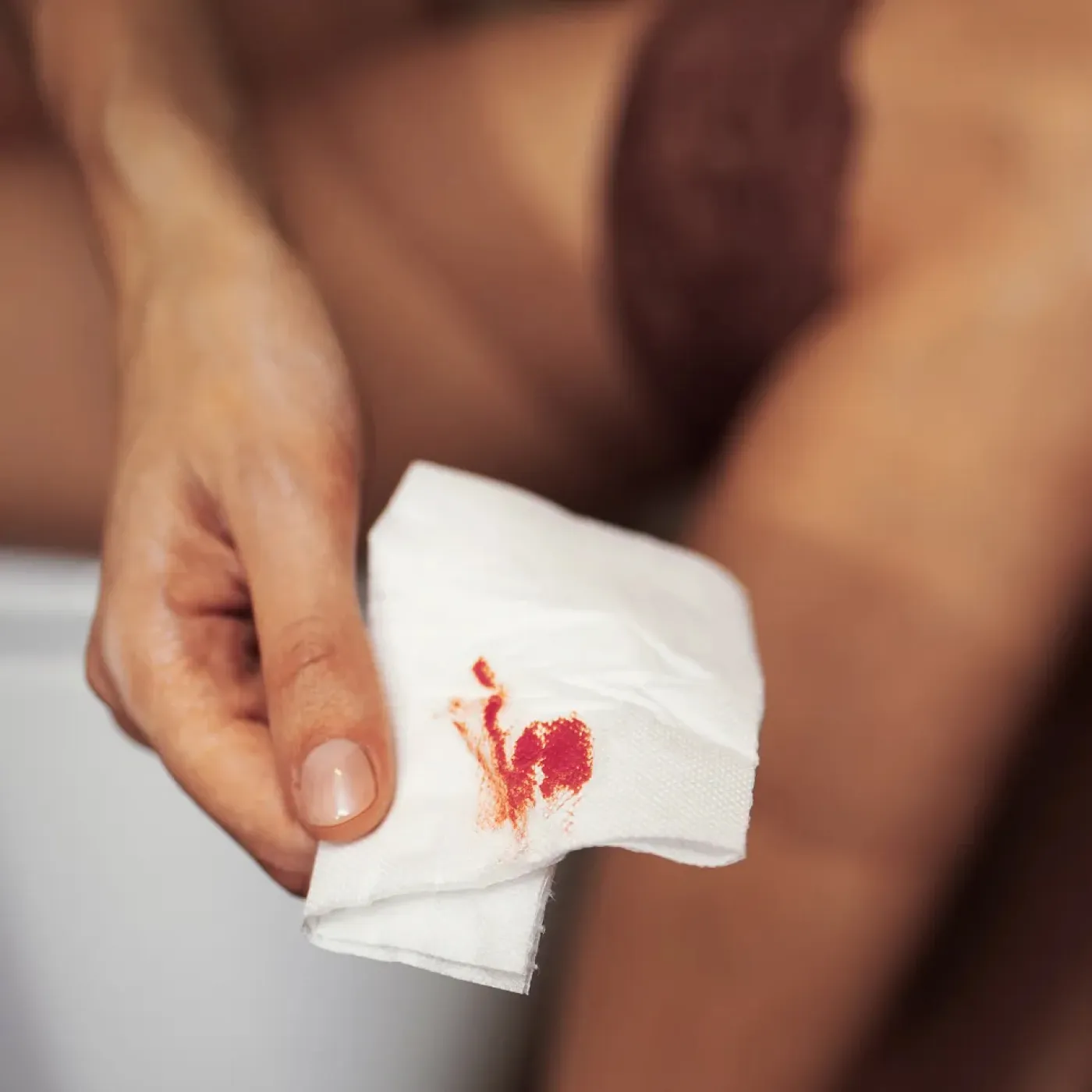
It can feel like a sudden, sharp pain…almost like a paper cut…but in the worst place possible (your anus). Then, you wipe and see bright red blood.
That combination of pain and bleeding can feel scary. But most of the time, the cause is something common and treatable like an anal fissure. Fissures are especially common if you’re dealing with constipation, high stress, pelvic floor tension, or even medications like Accutane. All of these can make the sensitive anal tissue more vulnerable to tearing.
Most of the time, fissures heal on their own with a few small changes to your daily habits. But if yours doesn’t, or if it keeps coming back, pelvic floor physical therapy can be a highly effective and often overlooked treatment option.
Still, anytime you notice new anal pain or bleeding, it’s a sign your body needs attention. If symptoms persist or worsen, it’s always best to check in with your healthcare provider.
What is an anal fissure?
An anal fissure is a small tear in the delicate tissue that surrounds your anal opening. And when you poop, it causes bleeding and lots of pain.
Fissures can be acute, meaning the tear is new and the symptoms last for up to 6 weeks, or chronic. A chronic anal fissure is when healing takes longer than 6 weeks, or the tear keeps opening up.
When they happen, fissures most often occur at the top (towards the vaginal opening) or the bottom (near your tailbone) of your anal sphincter.
What are the symptoms of anal fissure?
The main symptoms of an anal fissure include:
- Bright red blood, which you may notice when you wipe, on your poop, or in the toilet bowl
- Sharp, intense pain during a bowel movement
- Pain that can last minutes to hours after a bowel movement
- A feeling of muscle tightness or spasm
The pain from a fissure is usually most noticeable during and immediately after you poop, but not randomly throughout the day.
What is an anal fissure vs. hemorrhoid?
While they both share symptoms like anal discomfort and bleeding, the main difference is in the cause. Here are the main differences between anal tissues and hemorrhoids:
Anal fissures
These are tiny tears in the lining of the anus. They usually cause sharp pain during and right after your bowel movement and are often triggered by hard or large stools.
Hemorrhoids
On the other hand, hemorrhoids are swollen veins in or around your anus that can sometimes itch or feel tender. But they may also not hurt at all. Internal hemorrhoids can bleed and may cause irritation or a feeling of fullness.
For any new anal pain or bleeding, it’s always best to see your healthcare provider. They can examine the cause of your symptoms and get you the right treatment quickly.
What causes an anal fissure?
Anal fissures usually happen when you have chronic constipation and pass a hard, bulky stool. The muscle around your anal opening can also have a hard time relaxing like it’s supposed to. When that muscle stays tight and stool is difficult to pass, the delicate skin can stretch and tear.
But you may also be more likely to get a fissure if you have:
- Frequent diarrhea, which can a persistent irritation to the tissues
- Recently given birth (things like pregnancy-related constipation, birth trauma, and low estrogen levels can leave you more at risk)
- Anal trauma (like can happen during anal sex)
- Pelvic floor muscle tension
- Certain medications (including Accutane)
When a fissure happens, the pain can cause your anal sphincter to tighten or spasm. And that tightening can restrict blood flow to the skin and muscles in the area, which slows healing. Less blood flow means that the fissure takes longer to heal. And when it’s not healed, the next bowel movement hurts again, and the cycle continues.
This is why an anal fissure keeps coming back for some people.
Can Accutane cause anal fissures?
It might. One of the ways that Accutane (isotretinoin) treats acne is by reducing excess oil production. But it doesn’t just dry out your face.
It’s well known to dry out skin and mucous membranes throughout your body, including your lips, nose, and eyes. It may also impact the lining of your anal canal.
Some research shows people taking isotretinoin can develop constipation, anal irritation, bleeding, and even anal fissures. And it’s even been linked to Inflammatory bowel disease (IBD).
Since dry anal tissues are more fragile, and if you’re also constipated and passing hard stool, it’s easier for a fissure to form.
If you’re on Accutane (or any other form of isotretinoin) and noticing pain or bleeding with bowel movements, it’s a good idea to bring up fissures with your healthcare provider so that they can help you manage your symptoms, and make sure nothing more serious is going on.
Luckily, these side effects usually improve after finishing the medication. And treatments like pelvic floor physical therapy can help!
How are anal fissures treated?
When you have an anal fissure, the main goal is to improve stool consistency and reduce muscle spasm so that your tissues can finally heal.
Lifestyle changes
This can be as easy as a few simple changes in your daily habits to help reduce irritation and give the tear a chance to close:
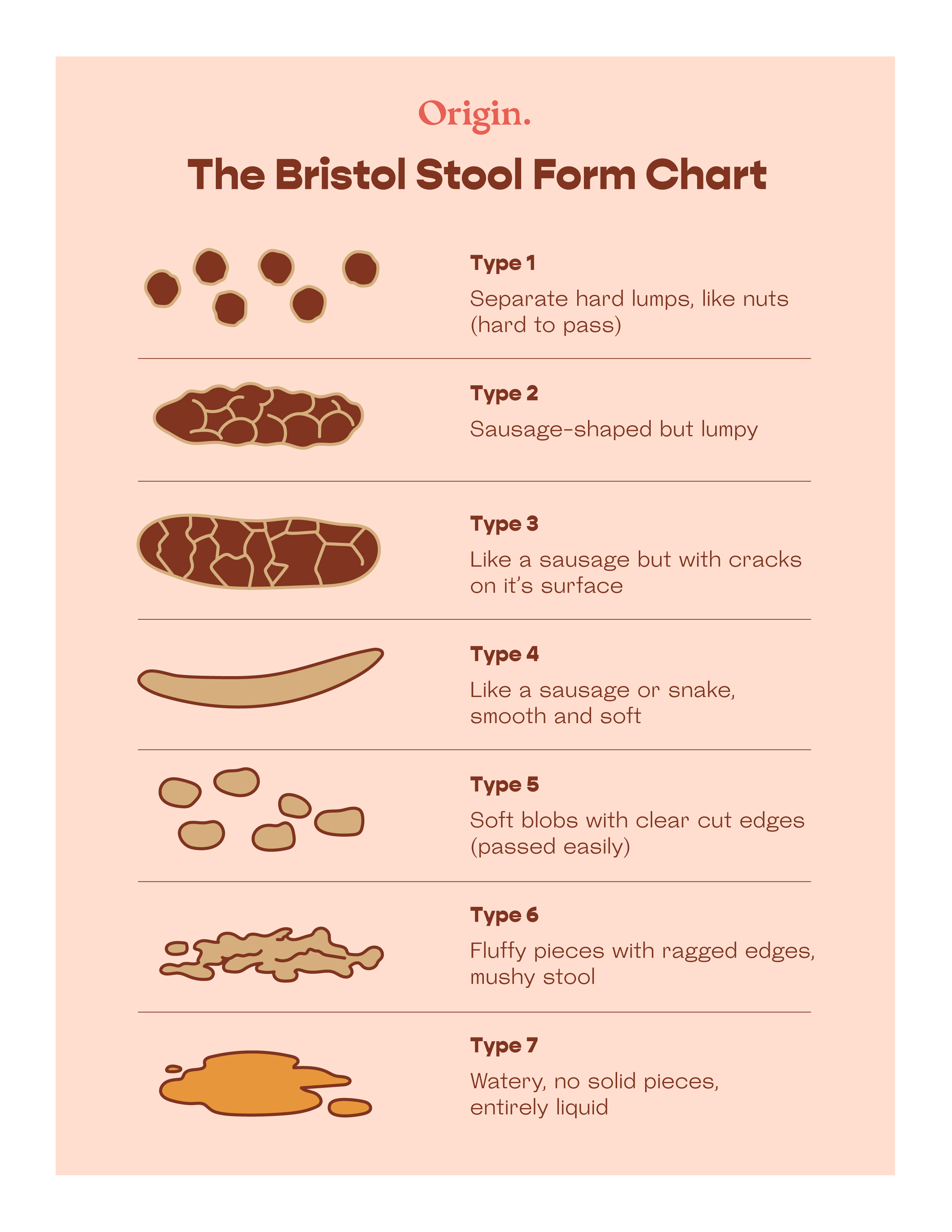
- Soften your stool: When you have a fissure, it can help if your stool is soft and easy to pass. Aim for stools that are a 4 or 5 on the Bristol stool chart below. Try increasing your daily fiber intake, drink plenty of water, and use stool softeners only when needed.
- Support healing tissues: Use a warm sitz bath for 10–15 minutes to ease pain and encourage healing. Avoid straining or sitting on the toilet for more than 10 minutes at a time.
Pelvic floor physical therapy treatment (yes, really)
You may not have realized it, but pelvic physical therapy (PT) can be a really helpful treatment option for anal fissures. Research shows pelvic floor PT can reduce pain, improve healing, and decrease recurrence rates for chronic fissures.
The main focus of treatment is to teach how to optimize your bowel function, and retrain your pelvic floor muscles so they can relax and lengthen properly when you poop.
Pelvic floor PT for anal fissures may include:
- A full assessment of your pelvic floor and anal muscles to better understand if they’re contributing to your symptoms
- Biofeedback, to help you understand how your pelvic floor muscles are working in real time
- Gentle manual therapy to reduce sphincter tension and lengthen scar tissue
- Breathing strategies to prevent straining
- Guidance on pooping mechanics and home exercises
Medical treatment for chronic fissures
If your fissure lasts longer than 6 weeks or keeps reopening, there are medications and other treatment options to help you heal:
- Prescription creams that have nitrates or calcium channel blockers are often prescribed to help relax your anal sphincter muscle and bring blood flow to the area
- Botox injections may be recommended to help with muscle relaxation
- A surgery called an internal sphincterotomy may be considered
Heal your anal fissure with Origin Physical Therapy
Anal fissures are common, painful, and frustrating, but pelvic floor physical therapy can help break the cycle of muscle spasm and pain.
At Origin Physical Therapy, our pelvic health PTs are trained to treat anal fissures with evidence-based, whole-body care. If you’re ready to feel better (and stop dreading the bathroom), book an evaluation and let us help you heal.
Sources
American Academy of Dermatology Association. “Isotretinoin: FAQs.” American Academy of Dermatology, www.aad.org/public/diseases/acne/derm-treat/isotretinoin/faqs. Accessed 2 Mar. 2026.
American Academy of Dermatology Association. “Isotretinoin: Side Effects.” American Academy of Dermatology, www.aad.org/public/diseases/acne/derm-treat/isotretinoin/side-effects. Accessed 2 Mar. 2026.
Bužinskienė, Dalia, et al. “Perianal Diseases in Pregnancy and After Childbirth: Frequency, Risk Factors, Impact on Women’s Quality of Life and Treatment Methods.” Frontiers in Surgery, vol. 9, 2022, article 788823. DOI: 10.3389/fsurg.2022.788823.
Gerbasi, Lauren, and John V. Ashurst. “Anal Fissures.” StatPearls, updated 15 Sept. 2025, StatPearls Publishing, 2025, www.ncbi.nlm.nih.gov/books/NBK526063.
Lu, Yi, and Alan Lin. “Lateral Internal Sphincterotomy.” JAMA, vol. 325, no. 7, 2021, p. 702. DOI: 10.1001/jama.2020.16708.
MedlinePlus. “Anal Fissure.” MedlinePlus, U.S. National Library of Medicine, medlineplus.gov/ency/article/001130.htm. Accessed 2 Mar. 2026.
van Reijn-Baggen, D. A., et al. “Pelvic Floor Physical Therapy in Patients with Chronic Anal Fissure: Long-Term Follow-Up of a Randomized Controlled Trial.” International Journal of Colorectal Disease, vol. 38, no. 1, 2023, article 3. DOI: 10.1007/s00384-022-04292-7.
“Anal Fissure – Expanded Information.” American Society of Colon and Rectal Surgeons, imis.fascrs.org/PortalTest/PortalTest/Patients/Diseases-and-Conditions/A-Z/Anal-Fissure-Expanded-Information.aspx. Accessed 2 Mar. 2026.
“Anal Fissure.” Forum Dermatologicum, journals.viamedica.pl/forum_dermatologicum/article/view/105423. Accessed 2 Mar. 2026.