Pelvic floor dysfunction affects millions of people across all genders and life stages, but it's widely underdiagnosed and undertreated. Whether your symptoms show up as leaking, pelvic pressure, pain, or bowel changes, they're not something you have to accept as normal. Pelvic floor physical therapy is the first-line treatment, and it works.
The pelvic floor is one of those parts of the body that most people don’t think about until something goes wrong. Whether you're leaking urine when you sneeze, feeling heaviness in your pelvis, or even experiencing low back or hip pain, these symptoms can feel isolating and impact you doing the things you love. However, we shouldn’t label these symptoms as normal or dismiss them just because they aren’t always talked about. This blog will walk you through what the pelvic floor is, what happens if it’s not working properly, who’s affected by pelvic floor dysfunction, and what you can do about it.
What is the pelvic floor?
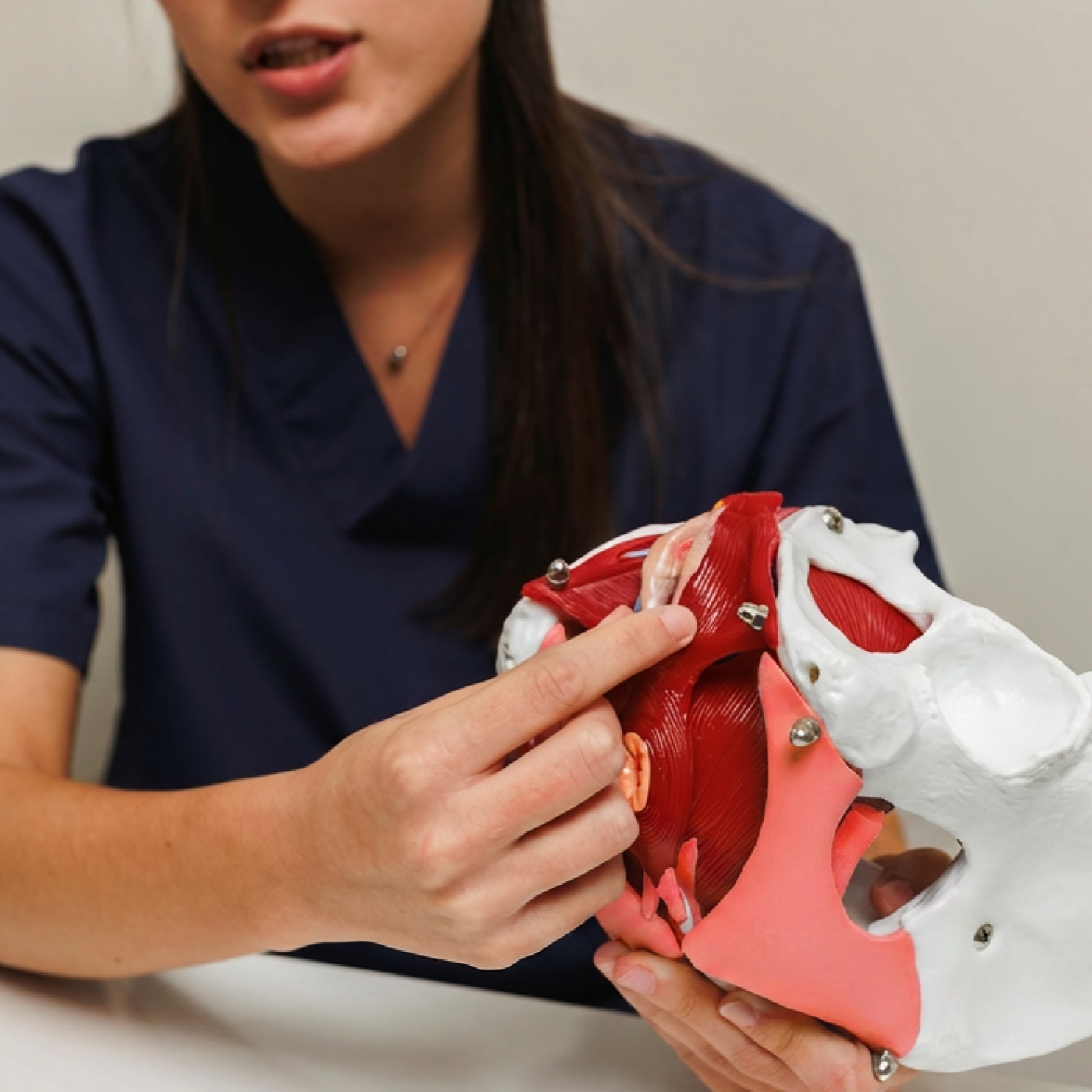
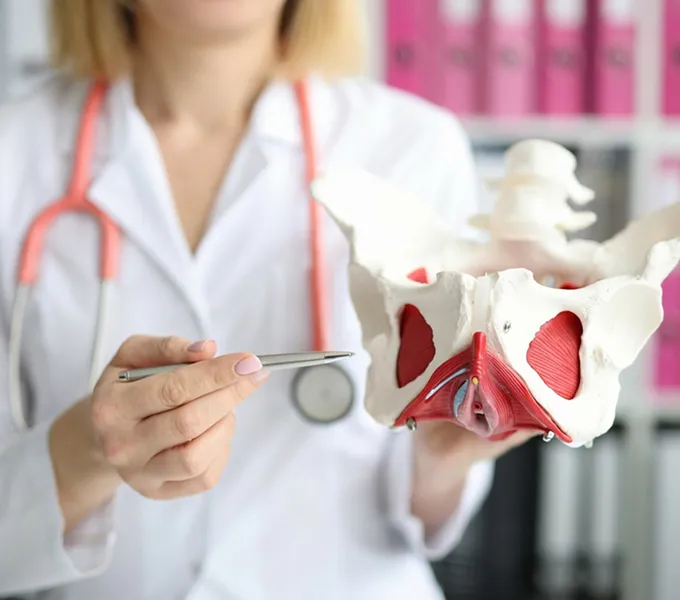
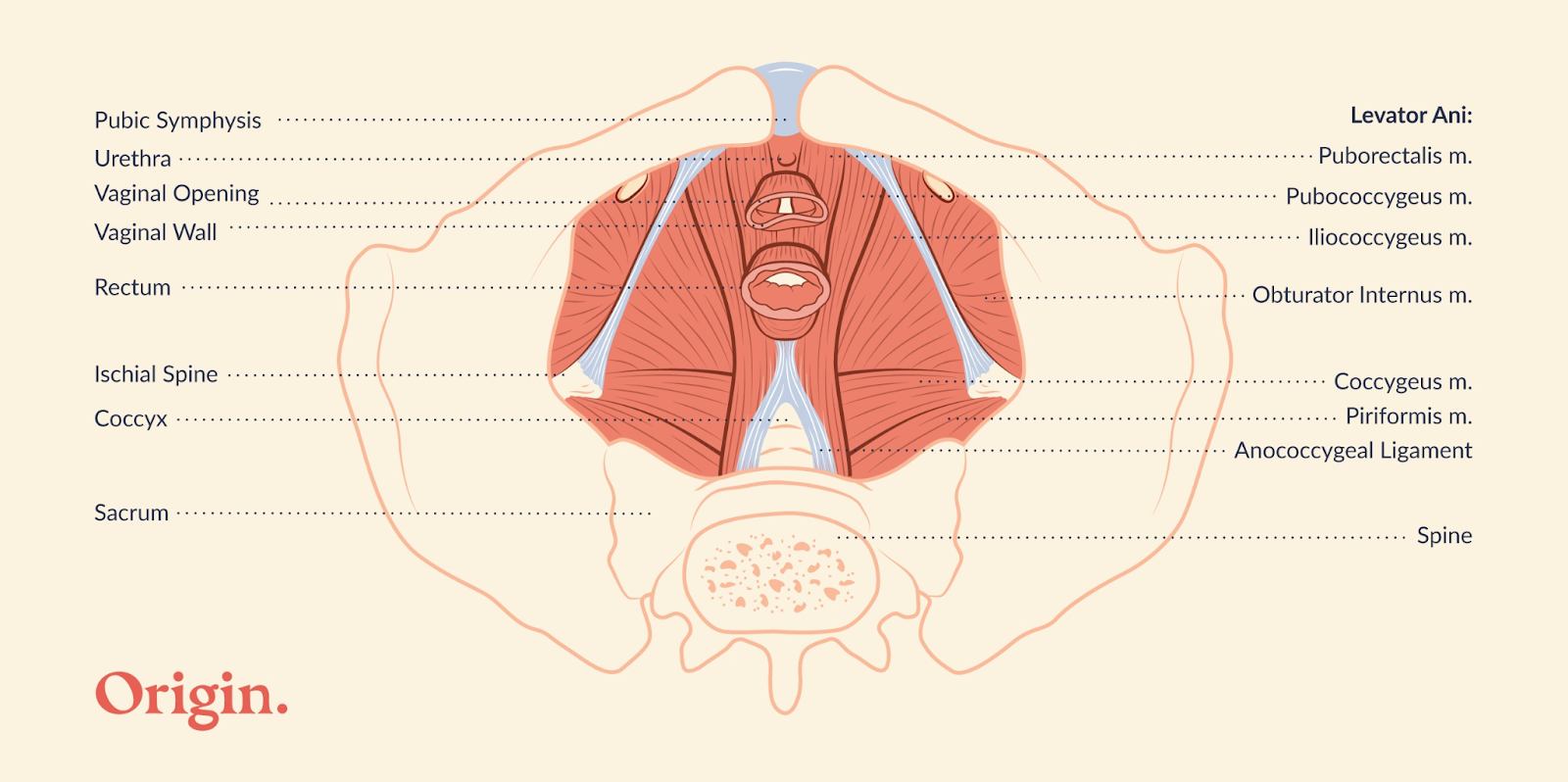
The pelvic floor is a group of layered muscles and connective tissue that spans the bottom of the pelvis, forming a supportive “hammock” for the bladder, rectum and reproductive organs (uterus, testes and prostate). When these muscles are strong and coordinated, they do a great job performing their 5 main functions:
- Stability (works with your abdominal and hip muscles to help you move)
- Support (for your organs)
- Sphincteric (hold back urine, gas, stool)
- Sexual (relaxes for penetrative intercourse and contracts during orgasm)
- Sump Pump (helps get fluid from legs back to the heart)
What is pelvic floor dysfunction?
Pelvic floor dysfunction (PFD) is an umbrella term that describes problems with how the pelvic floor muscles work. While many people think PFD is due to pelvic floor muscle weakness, it can also occur if the muscles are too tight and can’t relax properly or if they don’t coordinate well, meaning they don’t contract or relax at the right times.
Here are some common warning signs of pelvic floor dysfunction:
Pelvic floor dysfunction is remarkably common. Studies found that about 32% of women and 16% of men are affected by at least one symptom of pelvic floor dysfunction. Urinary incontinence alone is also widespread, reported anywhere from 56-63% of women and up to 32% of men. Yet people (healthcare providers included) will often brush these symptoms off as “normal aging” or “just part of life after childbirth,” which can prevent people from seeking help for conditions that are highly treatable.
Who experiences pelvic floor dysfunction?
While pelvic floor dysfunction can happen to anyone with a pelvis, certain life stages and circumstances can increase the risk:
- Pregnancy and postpartum: About 49% of people experience pelvic floor dysfunction during pregnancy or after birth.
- Perimenopause and menopause: Around 64% of postmenopausal women report urinary leakage.
- After prostate surgery: Up to 69% of men experience urinary leakage following prostatectomy.
- High-intensity athletics: Urinary leakage affects about 14% of male and 45.1% of female athletes in high-impact sports.
- Aging: About 37% of women 60-79 years old and 50% of women >80 years old report at least one symptom of pelvic floor dysfunction. Up to 40% of men over the age of 50 have symptoms of urinary frequency, urgency, or weak urine stream.
- Other risk factors: Overweight/obesity, chronic constipation, and chronic pain.
These numbers are staggering, however it may not be the full picture. This data is mostly based on people disclosing this information. For many people there is shame or embarrassment surrounding symptoms related to pelvic floor dysfunction and they may not be comfortable sharing their symptoms. Remember: even if you belong to one or more of these categories and you experience symptoms of pelvic floor dysfunction, you don’t have to “just live with it”. Origin can help. Make an appointment today!
What are treatment options?
While these symptoms are common and can be quite frustrating, pelvic floor dysfunction is totally treatable. Pelvic floor physical therapy is the first-line treatment for most pelvic floor disorders for people of all genders. Pelvic floor physical therapy can help you restore the balance of strength, flexibility, and coordination in your pelvic floor muscles to reduce or even completely resolve symptoms of pelvic floor dysfunction.
Pelvic floor physical therapy is highly individualized and a pelvic floor physical therapist can help determine the specific care that you need. Typically, pelvic floor physical therapy can include the following:
- Exercises to help strengthen, relax, or improve the coordination of the pelvic floor muscles
- Pain or tension relief using breathing techniques, manual therapy, and stretches
- Education on small habit changes to prevent symptoms from coming back
You don’t have to live with symptoms of pelvic floor dysfunction forever, and you don’t have to figure it out on your own. Origin offers in-person, virtual, and hybrid options for pelvic floor physical therapy, so you can get the care you deserve on your schedule. Schedule an appointment today!
Sources
Che, Raymond, et al. “Post-Pandemic Prevalence of Urinary Incontinence among Women in the United States and Associated Risk Factors.” International Urogynecology Journal, vol. 37, no. 3, 13 Oct. 2025, pp. 583–595, https://doi.org/10.1007/s00192-025-06280-1. Accessed 30 Apr. 2026.
Grimes, W. R., and Michael Stratton. “Pelvic Floor Dysfunction.” PubMed, StatPearls Publishing, 26 June 2023, www.ncbi.nlm.nih.gov/books/NBK559246/.
Helfand, Brian T., et al. “Prevalence and Characteristics of Urinary Incontinence in a Treatment Seeking Male Prospective Cohort: Results from the LURN Study.” The Journal of Urology, vol. 200, no. 2, 1 Aug. 2018, pp. 397–404, pubmed.ncbi.nlm.nih.gov/29477718/, https://doi.org/10.1016/j.juro.2018.02.075.
Kenne, Kimberly A., et al. “Prevalence of Pelvic Floor Disorders in Adult Women Being Seen in a Primary Care Setting and Associated Risk Factors.” Scientific Reports, vol. 12, no. 1, 14 June 2022, https://doi.org/10.1038/s41598-022-13501-w.
Mazur-Bialy, Agnieszka, et al. “Physiotherapy as an Effective Method to Support the Treatment of Male Urinary Incontinence: A Systematic Review.” Journal of Clinical Medicine, vol. 12, no. 7, 27 Mar. 2023, p. 2536, pubmed.ncbi.nlm.nih.gov/37048619/, https://doi.org/10.3390/jcm12072536.
Nygaard, Ingrid. “Prevalence of Symptomatic Pelvic Floor Disorders in US Women.” JAMA, vol. 300, no. 11, 17 Sept. 2008, p. 1311, https://doi.org/10.1001/jama.300.11.1311.
Palmieri, Stefania, et al. “Prevalence and Severity of Pelvic Floor Disorders in Pregnant and Postpartum Women.” International Journal of Gynecology & Obstetrics, vol. 158, no. 2, 4 Dec. 2021, https://doi.org/10.1002/ijgo.14019.
Rocío Adriana Peinado‐Molina, et al. “Pelvic Floor Dysfunction: Prevalence and Associated Factors.” BMC Public Health, vol. 23, no. 1, 14 Oct. 2023, bmcpublichealth.biomedcentral.com/articles/10.1186/s12889-023-16901-3, https://doi.org/10.1186/s12889-023-16901-3.
Rodríguez-López, Elena Sonsoles, et al. “Prevalence of Urinary Incontinence among Elite Athletes of Both Sexes.” Journal of Science and Medicine in Sport, vol. 24, no. 4, Apr. 2021, pp. 338–344, https://doi.org/10.1016/j.jsams.2020.09.017.