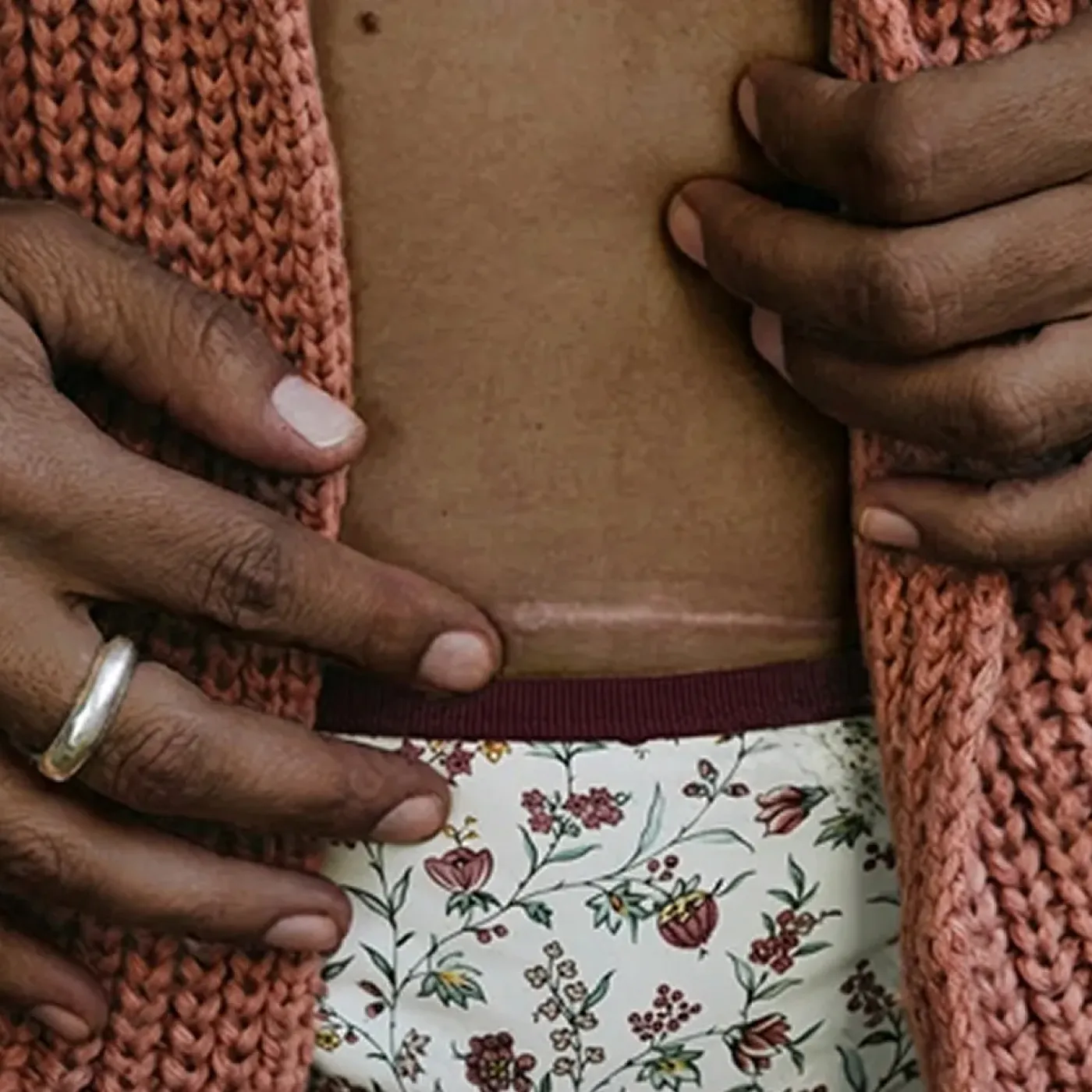
If you’ve noticed numbness, tingling, or strange sensations around your c-section scar, you’re not alone! While most conversations around c-section recovery focus on pain and healing, nerve-related symptoms often go unexplained and can leave you feeling confused or concerned.
It’s important to know that these altered sensations around your scar sensations are common, and there are ways to support your body’s healing and feel more like yourself again. Read on as we discuss why c-section nerve pain happens, and what you can do to alleviate it.
What happens to nerves during a c-section
As the most common surgical procedure in the US, cesarean sections (c-sections) are just that: surgery. During a c-section, a surgeon carefully cuts through and opens seven different layers of tissue, including skin, fascia, abdominal muscle, and uterine layers. Surgeons always do their best to avoid damaging nerves; however, nerve damage and entrapment can still happen.
What is nerve entrapment?
Post-surgical nerve entrapment occurs when a nerve is cut and trapped within a closed incision or when it is caught in scar tissue around an incision. Entrapment can compress the nerve and cause neuropathy, meaning your nerves send different sensory signals to your brain. Light touch might be painful, you might feel a burning sensation near scars or over them, or you might feel numbness or no obvious entrapment symptoms at all.
Nerve entrapment affects up to 30% of patients after any surgery. However, nerve entrapment is especially common for procedures that use the Pfannenstiel incision (the most common c-section incision type). C-sections can affect a few different nerves that run and work closely together, including:
- The ilioinguinal nerve, which provides sensation to your lower belly and upper thigh, and supplies some abdominal muscles
- The iliohypogastric nerve, which passes through your lower abdominal muscles, supplying them and giving them sensation
- The genitofemoral nerve, which helps provide sensation in your genital region and upper thigh
Is numbness after c-section normal? Common nerve sensations after a belly birth
Nerve entrapment can cause a whole host of sensations around your scar and the surrounding areas. While uncomfortable, these sensations are common and don’t need to cause serious alarm. However, that doesn’t mean you have to just deal with them! Pelvic floor physical therapy (PFPT) can help improve your nerve symptoms, whether they’re brand new or chronic, and ensure your whole body is recovering from surgery.
Nerve sensations you may feel after a c-section include:
- Numbness: You may experience a lack of sensation or total skin numbness after surgery, often around your scar and lower belly.
- Pain: Pain can feel sharp or like a burning sensation, and can radiate outwards to your sides and back. These feelings can start right after surgery, or occur much later if more scar tissue forms.
- Tingling: You may feel a tingling or a pins-and-needles sensation around your belly or upper thighs.
- Hypersensitivity: Things that don’t usually feel painful, such as a shower or the waistband of your favorite sweatpants, can start causing pain. Called allodynia, hypersensitivity can happen even if you’re experiencing numbness in the affected area.
Most people who have a c-section will experience some or all of these symptoms for a short while after their surgery; they aren’t always a sign of nerve entrapment. Ideally, these symptoms gradually improve as you recover and rehab after birth. However, if they stick around for many weeks after delivery, it’s possible you’re experiencing symptoms of post-surgical nerve entrapment that will benefit from medical care.
When to seek medical attention
While nerve pains such as numbness and tingling don’t always indicate serious problems, there are a few signs to watch out for during your recovery. Reach out to your healthcare provider right away if you experience any of the following:
- Fever
- Chills
- Severe swelling, pain, and/or redness in your arms or legs
- Heavy vaginal bleeding
- Worsening pain
- Shortness of breath
- Draining or leakage from the incision
How to improve nerve pain after c-section
Besides being uncomfortable, post-c-section nerve pain can leave you feeling frustrated and unfamiliar with your postpartum body. Numbness, burning, and tingling around the scar are common; however, they don’t need to be your permanent new normal! Physical therapy can help improve your c-section nerve pain.
While newer scars respond more quickly to physical therapy (typically improving in one to three months), it’s critical to let your c-section scar heal before you begin using the techniques listed below. Before you start these techniques at home, your incision should be healed and no longer scabbing.
If you start seeing a pelvic health physical therapist in the early weeks after delivery, your clinician may teach you how to perform variations of these techniques safely before 6 weeks postpartum. If you have not been specifically instructed by your PT or OB-GYN, however, do not start them before 6 weeks postpartum. Stop massaging your scar if you experience severe pain, shortness of breath, lightheadedness, or anxiety, or if your scar reopens during massage.
With that in mind, let’s discuss the techniques that can help with nerve pain and numbness after cesarean births.
Sensory re-education
After a serious surgery such as a c-section, the signals that your nerves send to your brain can become confused. Low-level stimuli, such as a light touch or a warm shower, can cause pain or tingling…even if your skin feels numb. Slowly introducing new sensations to the skin around your scar can help your brain desensitize the area and gradually increase your tolerance to rougher textures.
To desensitize your scar, begin by lightly brushing the area with a cotton ball or the tips of your fingers (wash your hands first!). When this becomes comfortable, move on to gently rubbing or brushing your skin with slightly rougher textures, such as a soft cloth or a paper towel.
C-section scar massage
You already know that a c-section will leave a scar and cause scar tissue to form. Scar tissue can contain adhesions, or areas where different tissues stick together where they shouldn’t. Nerves can get tangled up in adhesions and scar tissue, causing nerve pain or numbness after cesarean births. Here’s where massaging your c-section scar can help loosen things up, even if you’ve been dealing with discomfort for years.
Massaging and manually manipulating your scar (after your skin has become less sensitive to touch) can help remodel scar tissue and unstick any surface-level adhesions. Touching and mobilizing the skin makes the scar more flexible, helping it move, stretch, and feel sensations like the rest of your skin.
Additional interventions
Besides manual scar mobilization, your physical therapist may suggest heat therapy, cupping, or cold laser therapy to help with scar pain and stiffness. Some physical therapists are trained in dry needling techniques, which may support pain reduction, improve mobility, and address nerve-related symptoms around a C-section scar. Origin doesn’t shy away from full-body fourth-trimester care, and one of our expert clinicians can guide you through physical therapy to help improve your scar and c-section surgery pain.
How pelvic floor therapy can help c-section nerve pain
Pelvic floor physical therapy (PFPT) may seem like an obvious choice after a vaginal delivery; however, it’s just as helpful (if not more!) after a c-section. Working with a pelvic floor physical therapist is a proactive way to promote your recovery and prevent ongoing nerve pain, rather than “waiting to see” or responding to symptoms when they arise.
A pelvic floor physical therapist can work with you to:
- Desensitize and mobilize your scar: This not only helps to improve nerve pain by breaking up adhesions, but can also help prevent the c-section shelf (when skin hangs over a c-section scar).
- Strengthen your core muscles: Your abdominal muscles get cut and stretched during a c-section, and retraining them is key to recovery. PFPT involves gentle core exercises that help keep your trunk and low back supported and stable.
- Increase your mobility: Mobilizing your abdominal fascia, through exercises such as cat/cow and trunk rotations, can help loosen tissues that can contribute to nerve pain and overall stomach discomfort after c-section.
- Improve your posture: Low back pain is common during pregnancy and after delivery, whether vaginal or c-section. A pelvic floor physical therapist can work to correct your posture, which can help relieve low back pain, avoid nerve irritation, and keep your body functioning as a whole.
Dealing with nerve pain and numbness around your c-section scar can be overwhelming, but you don’t have to work through it on your own. Our pelvic floor physical therapists are here to help you prevent or improve nerve-related symptoms, no matter how long you’ve dealt with them. Reach out to schedule your evaluation today.
Sources
Sung, Sharon, and Heba Mahdy. “Cesarean Section.” National Library of Medicine, StatPearls Publishing, 2023, www.ncbi.nlm.nih.gov/books/NBK546707
Charipova, Karina, et al. “A Comprehensive Review and Update of Post-Surgical Cutaneous Nerve Entrapment.” Current Pain and Headache Reports, vol. 25, no. 2, Feb. 2021, https://doi.org/10.1007/s11916-020-00924-1. Accessed 7 July 2021
Elsakka, Khaled M., et al. “Ilioinguinal Neuralgia.” PubMed, StatPearls Publishing, 2020, www.ncbi.nlm.nih.gov/books/NBK538256
Centers for Disease Control and Prevention. “Urgent Maternal Warning Signs.” Centers for Disease Control and Prevention, 17 Sept. 2020, www.cdc.gov/hearher/maternal-warning-signs/index.html
He, Yusi, and Peggy Y. Kim. “Allodynia.” PubMed, StatPearls Publishing, 2020, www.ncbi.nlm.nih.gov/books/NBK537129
Poole, Judith H. “Adhesions Following Cesarean Delivery: A Review of Their Occurrence, Consequences and Preventative Management Using Adhesion Barriers.” Women’s Health, vol. 9, no. 5, Sept. 2013, pp. 467–477, https://doi.org/10.2217/whe.13.45
Wasserman, Jennifer B., et al. “Chronic Caesarian Section Scar Pain Treated with Fascial Scar Release Techniques: A Case Series.” Journal of Bodywork and Movement Therapies, vol. 20, no. 4, Oct. 2016, pp. 906–913, https://doi.org/10.1016/j.jbmt.2016.02.011
Chia, Yuan-Yi, et al. “Risk of Chronic Low Back Pain among Parturients Who Undergo Cesarean Delivery with Neuraxial Anesthesia: A Nationwide Population-Based Retrospective Cohort Study.” Medicine, vol. 95, no. 16, 1 Apr. 2016, p. e3468, pubmed.ncbi.nlm.nih.gov/27100449/, https://doi.org/10.1097/MD.0000000000003468